Our Pharmacy
Neurology Consultants of Dallas is now offering an in-house pharmacy to better serve prescription needs. The NCDRx Pharmacy serves the patients of Neurology Consultants of Dallas to provide a whole health experience.
Our pharmacy staff is an extension of the care team at Neurology Consultants of Dallas, allowing the medical staff to provide pharmaceutical services that answer the complex clinical and financial needs of NCD patients. Our pharmacy team knows that navigating insurance coverage and financial assistance for specialty medications is a confusing and stressful process, which is why our pharmacy staff completes all prior authorizations, billing and insurance paperwork. We also aid patients in connecting to financial assistance programs.
Patient convenience with easy access to the Rx care team, the neurologist and pharmacy staff
Increased quality of care and compliance, ensuring patient adherence.
Pick-up medication during the visit, minimizing patient wait times.
Fast and free delivery simplifies the refill process.


Meet the Pharmacist:
Vinika Amin is our Lead Pharmacist. Vinika grew up within the medical world, which gave her opportunities to see what it takes and feels like to serve in healthcare from a close quarter. While growing up, Vinika had a strong desire to help people within her community, and with that same intent, she chose pharmacy as her career option. Vinika gets immense gratitude and satisfaction while working for and with her patients. She started pursuing her pharmaceutical education by obtaining a bachelor’s degree in India and a master’s degree from Long Island University, NY. She continued to explore additional education by obtaining her doctorate in pharmacy from Nova Southeastern University, FL.
In Vinika’s free time, she finds cooking therapeutic and explores new flavors and cooking methods to bring out her creativeness in the kitchen!
Contact Info
NCDRx is currently serving patients of Neurology Consultants of Dallas. If you have questions, please contact us!
- Phone: 469-498-1710
- Toll Free: 877-460-3120
- Hours of Operation: 9:00 AM – 5:00 PM
- 8390 Lyndon B. Johnson Freeway, 1st floor, Suite 175, Dallas, TX 75243
Manage Your Healthcare needs.
Thank you for selecting NCDRx Pharmacy for your medication needs. With our in-house pharmacy services, you have a system of care that is centered around your prescription needs. It’s designed to enhance your therapy and help you achieve the best health outcomes. Equally important, you have a team of highly trained neurologists, pharmacists and caring staff to help walk you through every part of our process.
At the center of our pharmacy services is a team of highly trained and compassionate professionals led by an NCDRx Pharmacist. They are here to help should you need information about your condition, want guidance on how to safely take your medications, or need insurance claims assistance.
Service That Centers Around You
We offer personalized counseling that focuses on your prescription needs as well as the latest information to help you gain the most from your treatment. Equally important, should your course of treatment change, we are here to review the new medications with you and to assist you setting up a new schedule for taking them. If you have any questions, we are here to help with the following:
- Details on when you need to take your medication and the correct dosing
- Answers to any questions you might have
- Information on how to best manage any possible side effects
- Advice on how to best adhere to your treatment schedule as well as provide information on the correct treatment guidelines
- Details on how to use your medication safely and effectively.
- Our team is dedicated to helping you and your caregivers manage your medications
- Can help you understand how to take your medications safely and correctly
- Can help you manage side effects and the effectiveness of your medications
How to Use Our Services
Your provider will send the prescription to our specialty pharmacy. Our staff will begin the process of enrolling you in our specialized patient management program service that includes education about how and when to take your medication, how to manage potential side effects and ongoing clinical evaluation and support. Our specialty pharmacy’s patient management program is provided to you at no additional cost.
You may order refills by:
- Stopping by our specialty pharmacy located at 8390 LBJ Freeway Suite 175, Dallas, TX 75243.
- Calling our specialty team at: 469-498-1710 or Toll Free: 877-460-3120.
- Using your NCD Patient Portal to request a refill or medication change.
If you have lost your medication or supplies, or if you need your prescription(s) in advance of travel, please call our specialty pharmacy and our staff will work with you and your insurance company to ensure that your medications are covered and that there is no lapse in therapy.
Once the prescription is ordered and dispensed, it can be picked up at our Dallas office at: 8390 Lyndon B. Johnson Freeway, 1st floor, Suite 175, Dallas, TX 75243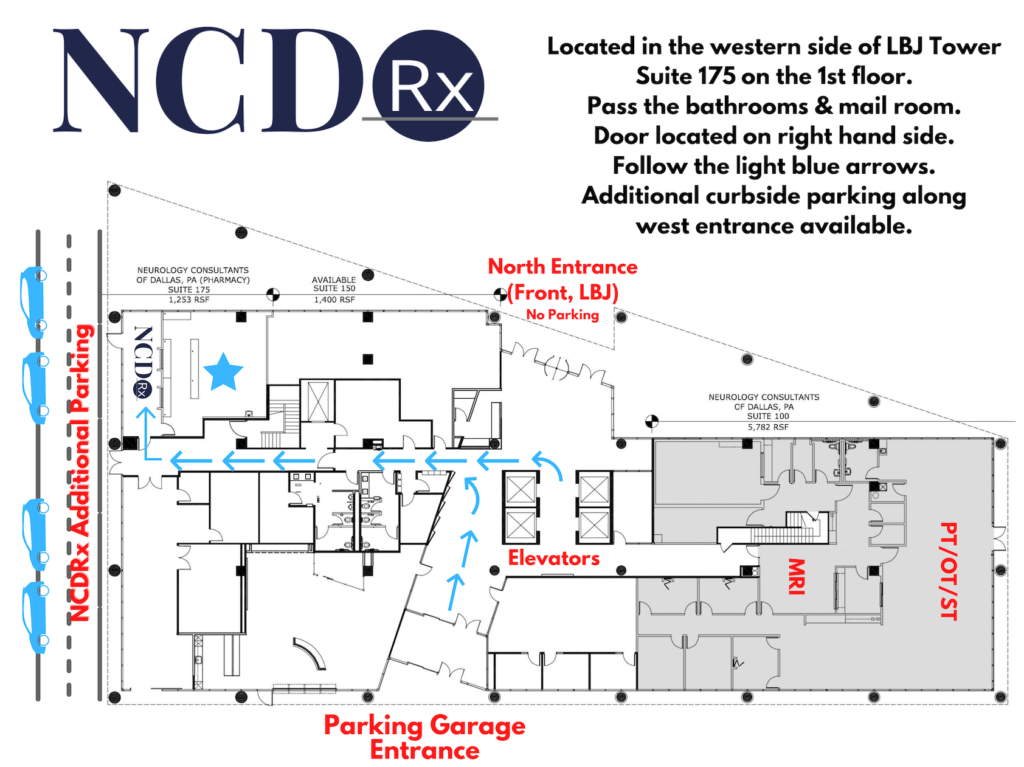
The patient can always pick up their medication(s) from our pharmacy or a free delivery to their home can be scheduled.
Insurance, Billing and Financial Assistance
Our team works with your insurance company to help get your specialty prescription covered. You may have to pay a copay each time a medicine is filled. We will tell you the exact amount you need to pay. The copay amount for a specialty pharmacy medication may still be high, despite having your insurance company pay for most of the cost. Our team will research various financial assistance programs available to possibly lower your medication therapy cost. We may ask you to fill out a patient medication assistance program authorization form in order to provide these services.
Some medicines need documentation for costs to be covered. This process is called prior authorization. Our team has the expertise to process this paperwork, which may take a few business days to complete. Our team keeps you and your doctor informed throughout the process, especially if there are expected delays. If insurance denies coverage for your medicine, our team can help your doctor file an appeal.
If your insurance plan considers our pharmacy an out-of-network pharmacy, we will inform you of the cost to fill your medicine with us. Our staff will transfer your prescription to an in-network pharmacy if there is a cost savings to you.
Any balances must be paid prior to your next refill. We accept credit/debit cards, cash, personal checks and most flexible spending accounts. If you get a check from your insurance company, you should send it to our specialty pharmacy with a copy of the Explanation of Benefits (also known as the EOB) statement you received. If you have any questions regarding this, please call us at: 469-498-1710 or Toll Free: 877-460-3120. If you need help arranging a payment plan for the balance you owe, we will be happy to help you set up a payment plan. Please call us to discuss your situation.
Frequently Asked Questions
Our specialty pharmacy can dispense for most insurance companies. Occasionally, your insurance company will require the use of another pharmacy for specialty medication needs. In these instances, we will transfer your prescription and have the new pharmacy contact you.
From time to time, it is necessary to substitute generic drugs for brand-name drugs. This could occur due to your insurance company preferring the generic be dispensed or to reduce your copay. If a substitution needs to be made, and after careful consideration by your caregiver/pharmacist team, a member of our pharmacy team will contact you prior to dispensing the medication to inform you of the substitution.
You should call our specialty pharmacy team if:
- Your address, telephone number or insurance information has changed.
- You have any questions regarding the status of your prescription.
- You have concerns regarding how to take your medication.
- You need to reschedule or check the status of your delivery.
- You need to start or stop a medication or if your dose changes.
- You have a reaction or allergy to your medicine.
- You would like additional information regarding your plan for therapy.
- You suspect an error in delivery or dispensing has occurred.
- You notice your medication has been recalled by the FDA.
- You should also contact us with any other questions or concerns. Our staff is happy to assist you with your specialty pharmacy needs, including:
- Helping you get access to medications during an emergency or disaster.
- Providing you with tools to manage your therapy, including educational materials and consumer advocacy support.
Yes. Follow your doctor’s instructions for both the amount of the medication you should take and the length of time you should take it. We understand that some medications may have unpleasant side effects or be difficult to take or give. Our pharmacists are available to offer practical advice about dealing with these issues and can help you contact your prescriber about the medical management of these side effects.
Contact Us
We’re here to answer any questions in order to make your appointment easier.
Find a Specialist
Learn more about our fellowship-trained specialists!
NCD Testing Center
Learn more about the testing available for seizures in our Neuro Testing Center.

